What is knee osteoarthritis?
Knee osteoarthritis is a degenerative joint disease characterized by the progressive deterioration of the articular cartilage, eventually leading to bone-on-bone contact. Common symptoms include joint pain, stiffness, a limping gait, and angular deformity of the lower limb, most commonly genu varum (inward angulation of the tibia).
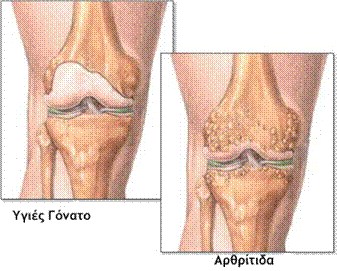
Knee osteoarthritis
How is knee osteoarthritis managed?
Initial treatment focuses on conservative management, including weight reduction, the use of analgesics and anti-inflammatory medications, activity modification to reduce joint stress, physical therapy, and walking aids such as canes.
When symptoms persist despite conservative measures and the patient’s quality of life is significantly affected, surgical intervention becomes indicated.
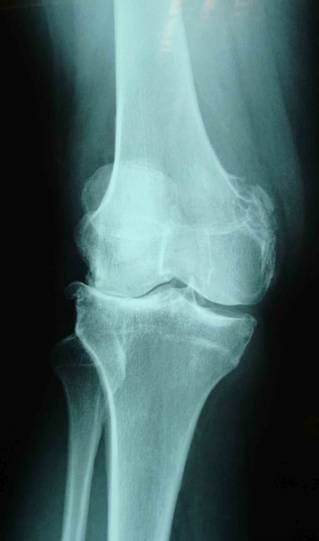
Severe knee osteoarthritis with varus deformity and bone-on-bone contact.
What is total knee arthroplasty (TKA)?
Total knee arthroplasty involves replacing the damaged joint surfaces with artificial components. During the procedure, the worn cartilage and a portion of the underlying bone from the femur and tibia are removed and replaced with metal prostheses of equivalent thickness. These metal components articulate with the aid of an intermediate high-density polyethylene insert. The prosthetic components may be fixed to the bone with or without bone cement. A hybrid technique is commonly used, involving cement fixation of the tibial component while allowing biological fixation of the femoral component, which is often coated to enhance bone integration.
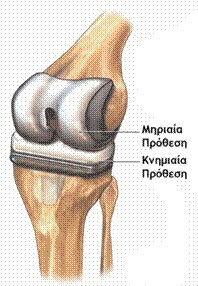
The total knee arthroplasty
What are the indications for total knee arthroplasty?
TKA is indicated in patients with advanced knee osteoarthritis and significant symptoms such as:
- Severe pain that limits work, recreational activities, and overall quality of life.
- Moderate to severe pain at rest, either during the day or night.
- Pain unresponsive to medications, physical therapy, or assistive devices.
- Stiffness resulting in significant restriction of knee mobility.
- Limb deformity.
- Adverse effects from prolonged medication use.
- Failure of conservative treatment.
Candidates are typically over 60 years of age and suffer from debilitating pain and functional limitations.
Knee osteoarthritis causes significant pain and dysfunction.
What are the goals of total knee arthroplasty?
The primary goals of TKA are to alleviate pain, restore joint function, and improve the patient’s quality of life. Postoperatively, patients can expect to resume normal daily activities, although high-impact or excessive physical stress is discouraged.
What are the alternative surgical options for knee arthritis?
In selected, less advanced cases, alternative procedures may include knee arthroscopy, synovectomy, or osteotomy. In severe cases, knee arthrodesis may be necessary.
What are the conservative (non-surgical) alternatives for managing knee osteoarthritis?
TKA is generally reserved for patients with chronic knee dysfunction and serves as a definitive treatment. In patients with milder symptoms, the following measures are recommended:
- Weight loss
- Reduction or modification of physical activity
- Analgesic and anti-inflammatory medications
- Physical therapy
Is it advisable to postpone total knee arthroplasty as much as possible?
This notion is incorrect. Early surgical intervention can yield better functional outcomes. Delaying the procedure may compromise pre- and postoperative quality of life. Since osteoarthritis is a progressive condition without a curative conservative treatment, postponing surgery may result in undergoing the procedure at an older age with potentially more complications.
What should patients expect from total knee arthroplasty?
TKA achieves significant pain relief in approximately 95% of patients. It allows resumption of daily activities and, under certain conditions, even participation in some sports. Most patients regain much of the mobility they had lost.
What components and materials are used in total knee arthroplasty?
A TKA implant consists of:
A femoral component
A tibial component
A polyethylene insert between them
A patellar component resembling a button
The metallic parts are typically made from titanium or cobalt-chromium alloys, while the plastic parts are made from medical-grade polyethylene.
Various designs, sizes, and materials exist. In selected cases, custom-made implants tailored to the patient’s anatomy can be utilized.

The materials comprising total knee arthroplasty implants
What is the expected lifespan of a total knee prosthesis?
Prosthesis longevity depends on material wear resistance (especially polyethylene), level of physical activity, bone quality, and other factors. While statistical data show survival ranging from 1 month to 35 years, approximately 80% of knee replacements last for at least 20 years.
How soon after surgery can patients walk independently?
Recovery time varies depending on individual factors. Most patients are able to walk independently within 4 to 6 weeks postoperatively. Some, especially elderly patients, may require assistive devices like canes for a longer duration.
When is driving permitted after TKA?
Driving should be avoided for 4 to 6 weeks or until adequate control of the lower extremities is restored. The exact timing should be determined by the operating surgeon.
